Person-centered approaches with SafeSide CARE
Engage, unite, and support your workforce, helping diverse populations to think, act, and communicate with a common set of principles and best practices. SafeSide CARE is a suicide prevention workforce education program delivered through a structured, video-led InPlace® workshop, with ongoing learning and support over time.
SafeSide CARE is delivered through the InPlace® Learning model, which combines video-based teaching and demonstrations with group interaction. It fosters skill development in groups ranging from small teams to larger organizational units.
SafeSide CARE
SafeSide provides suicide prevention education for diverse workforces, bringing together both clinical and lived expertise. It begins with a structured, video-led InPlace® workshop where teams learn together, followed by ongoing access to learning, support, and updated resources to help apply these skills in practice. SafeSide CARE is for whole teams, including clinicians, non-clinical staff, and interdisciplinary services. Learn more about the delivery model here.
Mental Health
Suitable for: Psychiatrists, psychologists, counselors, social workers, and non-clinical colleagues, including peer workers.
Primary Health
Suitable for: General practice and community sector professionals.
Youth Services
Suitable for: Clinical and non-clinical roles, working with children and youth up to age 25.
Alcohol and Other Drugs
Suitable for: Counselors, allied health, social workers, and peer workers in Alcohol and Other Drugs services.
What Changes in Practice
SafeSide CARE supports teams to build confidence in responding to suicide concerns, use a shared approach to conversation, documentation and care planning, and apply more consistent care across services.
Confidence in responding to suicide concerns
Increased confidence, consistency, and quality in asking about suicide concerns, supported by a structured approach to understanding and responding to risk.
Hopeful experiences
Supports more recovery-oriented conversations, helping people feel heard, understood, and able to identify their own strengths and supports.
Support for Your Workforce
Helps staff navigate complex situations with greater clarity and consistency, supporting confidence, teamwork, and day-to-day practice.
Evidence behind SafeSide
The program and its adaptations are built on more than a decade of research and are continuously updated to incorporate the latest science, regulations, and suicide prevention practices.
of SafeSide CARE participants say they can apply the training in their job
of SafeSide CARE: Youth Services participants were confident in suicide prevention after the workshop.
Framework for Suicide Prevention: Overview and Evidence Summary
Evaluation of sustainable, blended learning workforce education for suicide prevention in youth services (opens in new tab)
Brief Video-Based Suicide Prevention Training for Primary Care (opens in new tab)
How SafeSide CARE Works
How SafeSide CARE Is Delivered
SafeSide CARE is delivered through a structured, video-led InPlace® workshop showcasing clinical and lived experience teachings where teams learn together through real-world demonstrations, guided discussion, and practical application of the SafeSide Framework.
Time Commitment
The initial workshop can be be completed within a half a day, with flexible delivery options to suit different service contexts.
Ongoing Learning
Ongoing access to live Questions and Updates sessions, a Community of Practice, weekly microlearnings, and updated resources supports teams to reinforce skills and maintain consistency over time, rather than relying on one-off training alone.
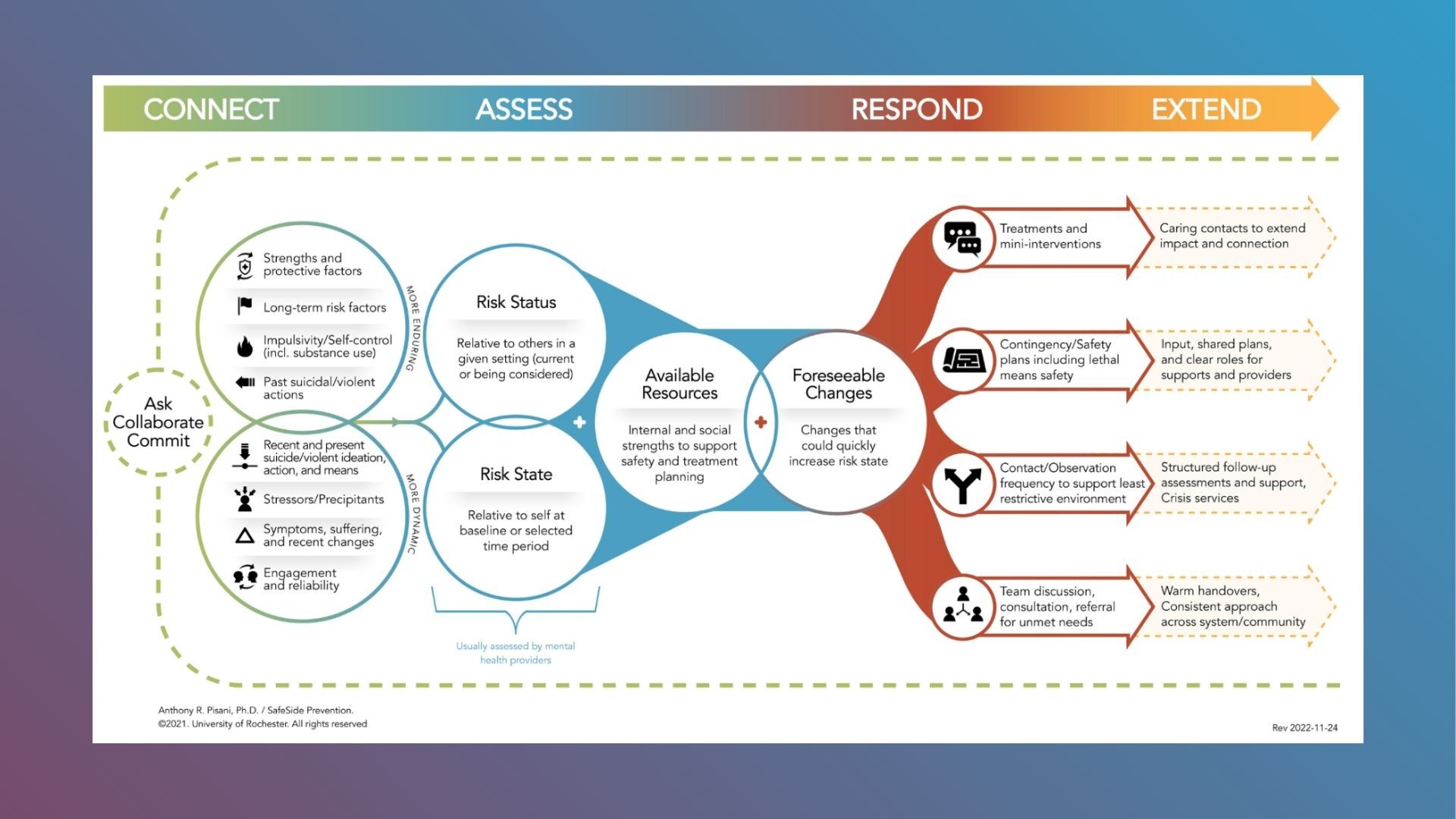
The SafeSide Framework
SafeSide CARE is built around the SafeSide Framework, which aims to enhance suicide prevention across all settings. It’s more than a set of steps; it builds common language and consistent practices for your people, no matter their role in prevention.
Better Together + Continuous Support
Lived Experience + Clinical Expertise
Expert clinicians and lived experience instructors co-led video-based modules and hold regular live, web-based sessions for feedback and ongoing support.
More than just a workshop
SafeSide CARE continues beyond the initial workshop, with ongoing learning and support embedded into everyday practice. With your subscription, you can access:
• Monthly Q&A sessions with experts to support application in practice.
• An online Community of Practice to connect with others using the SafeSide Framework.
• Up-to-date resources, including regular updates to tools, research, and strategies.
Frequently Asked Questions
Explore our FAQs for insights into SafeSide CARE
In InPlace® Learning, teams work through interactive video modules together with a nominated host from your organization who convenes the group. The content is embedded in the videos, so the host does not require specialized knowledge or training, thereby maintaining content fidelity throughout implementation.
Rather than just a one-off workshop, SafeSide embeds connection and interaction throughout their members’ learning journey through:
• Community of Practice where you can access tools and resources, and also ask questions of SafeSide faculty and peers worldwide.
• Weekly microlearnings delivered straight to your inbox.
• Access to exclusive SafeSide Live Learning sessions with clinical and lived experience faculty
SafeSide CARE focuses on building workforce capability in responding to suicide concerns through a common framework and ongoing learning. Other SafeSide programs focus on complementary areas such as building healthy resilient teams or supporting organisations shifting to restorative just and learning culture practices.
Absolutely. While SafeSide CARE offers a foundational approach to suicide prevention applicable across various settings, we also work closely with organizations to tailor the training content, ensuring it aligns with your team's unique challenges and needs.
Subscribers gain access to our video-based training year-round, monthly Q&A sessions with experts, and various tools and refreshers. Additionally, our team provides ongoing updates to ensure your practices remain at the forefront of suicide prevention research and guidelines.
We continuously update our programs based on the latest research, evolving best practices, and feedback from our global community of practitioners. This ensures that your training is always aligned with current standards in suicide prevention.
Lived experience is at the heart of everything we do at SafeSide. Our organization was founded on the collaboration between clinical and lived expertise and our core belief in “better together”. Lived experience is embedded in everything we do, from co-designing content to implementation and ongoing learning.